In about 1-2% of pregnancies, an incompetent or weakened cervix is the cause of a miscarriage. Almost 25% of second-trimester miscarriages are due to incompetent cervix. Today we are going to be talking about cervical incompetence and all the things you need to know about it, I am also going to show you the ultrasound, are you ready, let’s begin.
What is cervical incompetence?
Women with incompetent cervix experience preterm deliveries because their cervix is either too short or too weak to sustain a full-term pregnancy. In women with an incompetent cervix, the pressure from the growing fetus inside the uterus causes the cervix to open prematurely, leading to preterm delivery in the second trimester.
The pregnancy loss typically occurs between the 16th and 24th weeks of pregnancy most commonly between weeks 18 and 22.
Normally, prior to delivery, the cervix becomes softer, shorter and its walls begin to thin out. During labor, the cervix begins dilating along with the contractions. A fully dilated cervix of 10 cm allows the vaginal delivery of the baby.
What are the possible causes of Cervical incompetence?
In some cases, the exact cause of incompetent cervix is not known. Causes of cervical incompetence in pregnancy might include the following:
- Congenital abnormality in the cervix or uterus( Müllerian duct defects (eg, bicornuate or septate uterus)
- Exposure to a drug called DES (diethylstilbestrol) during pregnancy, which can result in an abnormality in the cervix of the female baby. Besides the cervix, abnormalities in the uterus may also be present. This drug is currently banned during pregnancy.
- Conditions like Ehlers-Dandos syndrome, in which the collagen in the cervix can get affected.
- Previous surgery carried out on the cervix like:
- Medical termination of pregnancy: During this procedure, the cervix may be manually dilated, which could result in incompetence during future pregnancies.
- Conization biopsy: In this procedure, a biopsy is obtained from the cervix in the form of a cone to diagnose for cervical cancer. Thus, there is a loss of cervical tissue, which could result in the incompetent cervix.
Risks for cervical incompetence.
You’re more likely to have this condition if:
- You’ve had cervical incompetence in your previous pregnancy,
- Your cervix was injured during a previous delivery or curettage (D&C) and/or is dilated.
- You’ve had, without any known cause, one or more second-trimester miscarriages.
- You’ve had one or more than one spontaneous preterm deliveries.
- You have a uterine abnormality (such as a bicornate uterus (congenital uterine anomaly).
- You’ve had a procedure such as a cone biopsy or LEEP done on your cervix.
- Your mother took the drug DES (diethylstilbestrol) while she was pregnant with you.
Related pregnancy posts.
Tips to survive and cope with a high-risk pregnancy.
Pregnancy symptoms for the third trimester.
11 items that you must have during pregnancy.
Sharing is caring!!!

Signs and symptoms of cervical incompetence.
You may have no symptoms at all, or between 14 and 20 weeks you begin to have mild symptoms such as these:
- Pelvic pressure
- Premenstrual-like cramping
- Backache
- Vaginal discharge that increases in volume or becomes wetter
- Vaginal discharge that changes from clear, white or light yellow to pink or tan
- Spotting (light vaginal bleeding)
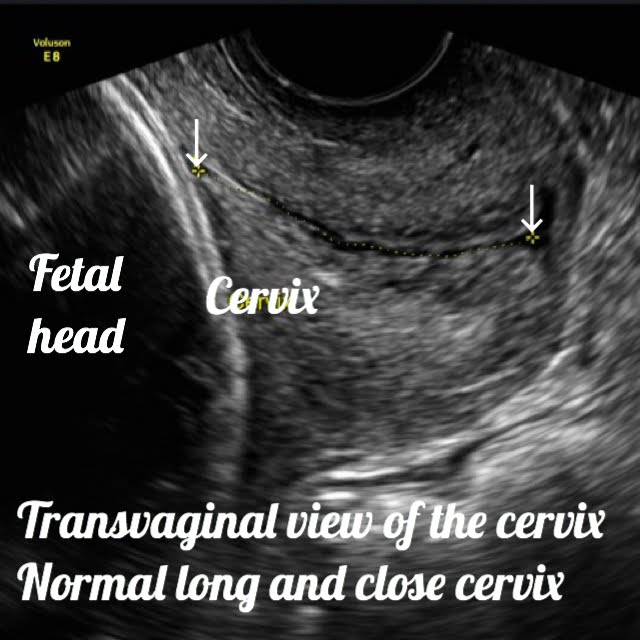
Incompetency of the cervix is generally not routinely checked during pregnancy, and wouldn’t be diagnosed until a miscarriage in the second or third trimester has occurred. But if you’re at risk for this condition, if you have any of the above symptoms or potential causes of incompetent cervix, your doctor may order regular transvaginal ultrasounds beginning at 16 weeks until 23 weeks to measure the length of your cervix and check for signs of early shortening.
If your cervix is found to be shorter than 25 mm or 2.5 cm, you’re at a much higher risk for preterm birth and therefore may need to go for treatment.
Treatment of Cervical incompetence.
- Bed Rest
- Steroids: To stop your cervix from dilating.
- And finally Cervical Cerclage
What is Cerclage for Cervical incompetence?
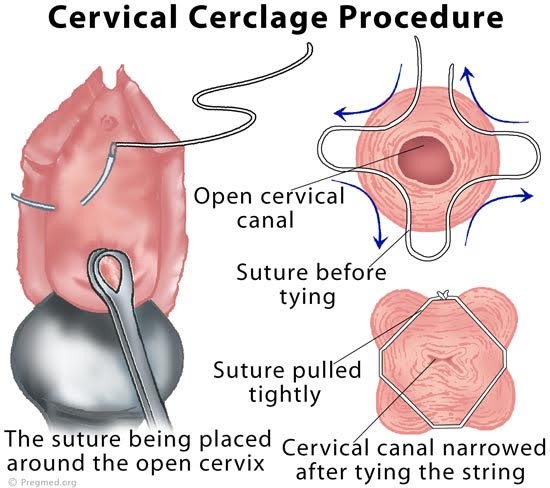
If you’re less than 24 weeks pregnant or have a previous history of early premature birth or if an ultrasound shows that your cervix is opening, your obstetrician may suggest a ‘cervical cerclage’. This procedure is usually performed between 4 to 16 weeks of pregnancy with spinal anesthesia.
Placement of a cerclage is the standard treatment for cervical insufficiency. A cerclage is the placement of a band or suture for reinforcement to help prevent the amniotic sac from “funneling” down into the cervix prematurely. There are different types of cerclage procedures, including transabdominal cervical cerclage and transvaginal cervical cerclage.
Between weeks 36-38 these sutures will then be removed to prevent any problems from occurring when you go into labor. Removal of the cerclage does not result in spontaneous delivery of the baby.
The success rate for cervical cerclage is supposed to be 80-90%.
Transvaginal ultrasounds for confirming a diagnosis of cervical incompetence.
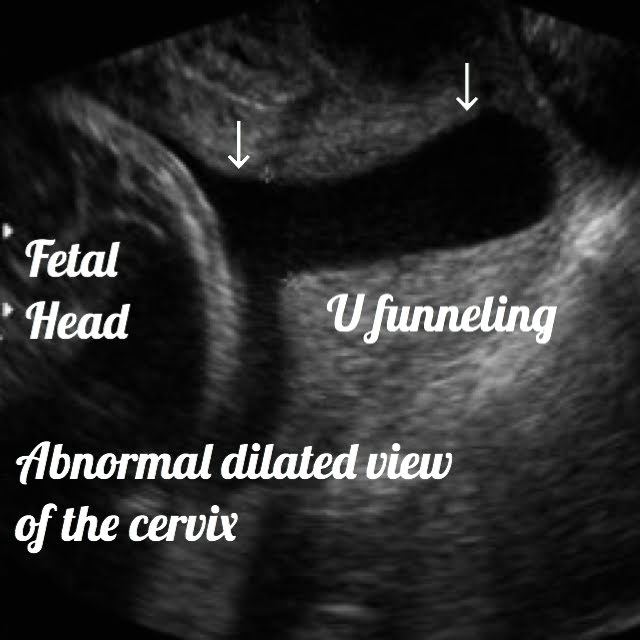
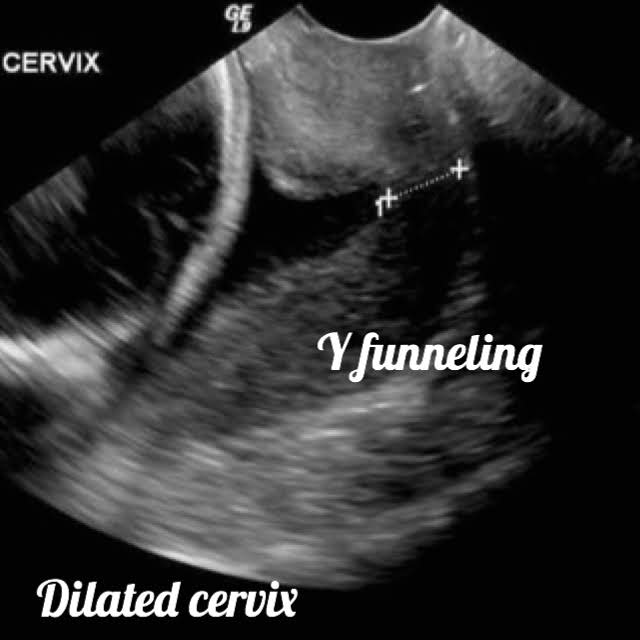
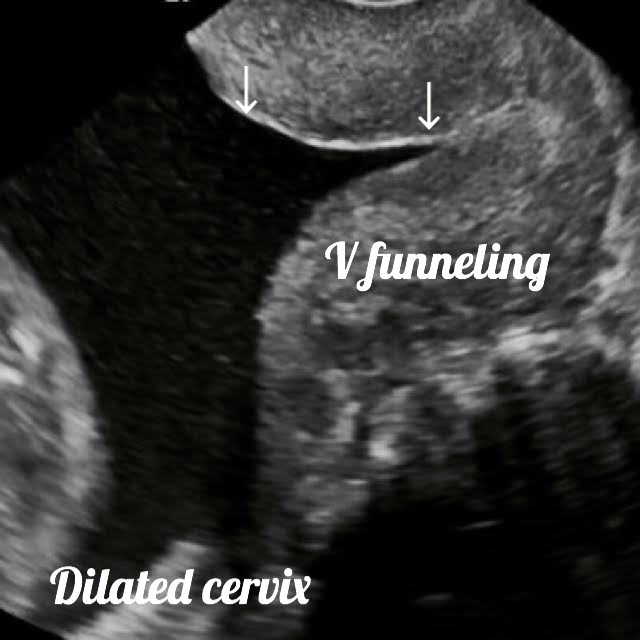
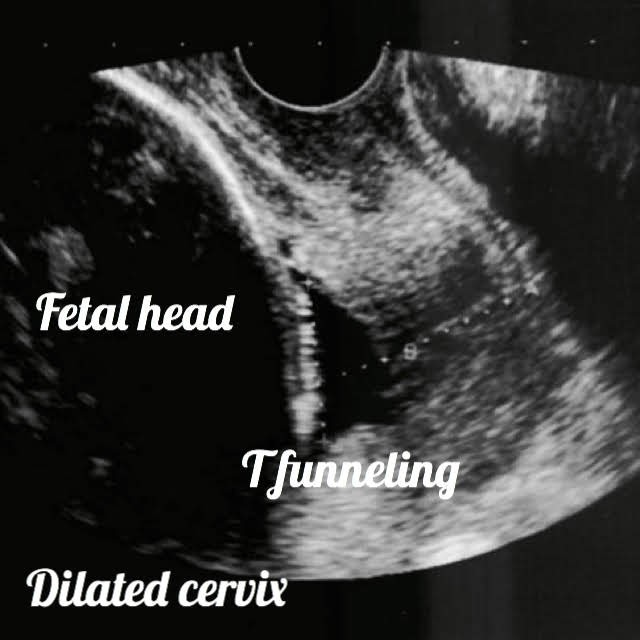
What is the meaning of Cervical funneling: CF is the opening of the internal cervical opening with protrusion of the amniotic sac into the cervical canal.
Cervical funneling can be assessed with either translabial or transvaginal scanning
Internal os may open and close in the absence of a palpable uterine contraction.
Shapes of CF are U, Y, V, or T.
Funneling is probably normal after 32 weeks.
Final words about Cervical incompetence.
There is nothing you can do to prevent cervical insufficiency or an incompetent cervix. Since the reasons are largely unknown, it is near impossible to come up with ways to prevent the complication from occurring. There is no way to detect an incompetent cervix until you are pregnant and the problem shows up. So you cannot even take preventive measures the first time around. However, if you know from a prior miscarriage or pregnancy that you have an incompetent cervix, your doctor will monitor you closely from the very start of your pregnancy, and somewhere around the end of your pregnancy first trimester or the beginning of your pregnancy second semester, you can get a cerclage to prevent the complications of incompetent cervix from showing up.
Zadi. xo
Disclaimer: Due to HIPPA regulations all patient information is protected on this site. The majority of the Ultrasound images are my own. The information provided on my blog is designed to provide helpful information about the topic. And this post is made with the best of my knowledge. Therefore, this post is not intended to diagnose or treat any medical condition. For diagnosis or treatments consult your own physician. The author is not responsible or liable for any mistreated pathologies.










This is a very helpful and informative explanation. Pregnancy loss is so tragic and heartbreaking, and there often are no answers. But what a comfort for those who can figure out the cause and prevent it from happening again.
I know a woman who lost two babies to preterm labor before the doctor discovered she had this issue (read her story here: https://mamarissa.com/karens-infant-loss-stories/). Thankfully, she went on to have several healthy children!
Hi Marissa, thanks for reading my blog today, I really appreciate your thoughts, I’ll take a look on your friend’s story, yes like you said pregnancy loss is a hard topic that unfortunately touches to a lot of us, I am glad I can help someone out there ?
Does having preterm labor indicate an incompetent cervix if they didn’t find any other specific reason causing early labor? At 28 weeks with twins I was fully effaced and started dilating, went into active labor and had them by 29.6. They are perfectly wonderful boys but I’m still so curious as to the why! My cervix had always measured nice and long previous
Hi dear, unfortunately there are many possible reasons for incompetent cervix but all of them remains hidden until it happens, and is also known that patients with multiple pregnancies have a higher chance of early labor and incompetent cervix, the only solution is a cerclage on your next pregnancy, and the specific answer for your question is Yes, you might have incompetent cervix, but don’t worry you will be fine next time, now the course of action is well known by your doctors so they’ll keep a close eye on you next time , I hope this helps
[…] All you need to know about Cervical incompetence during pregnancy. […]
Hello.This post was really fascinating, especially since I was investigating for thoughts on this topic last couple of days.
The next time I read a blog, I hope that it doesnt disappoint me as a lot as this one. I mean, I do know it was my option to read, however I truly thought youd have one thing fascinating to say. All I hear is a bunch of whining about something that you would fix for those who werent too busy on the lookout for attention.
I just like the valuable info you supply on your articles. I will bookmark your blog and test once more right here regularly. I am reasonably certain I?l learn plenty of new stuff right here! Best of luck for the following!
This is really interesting, You’re a very skilled blogger. I have joined your feed and look forward to seeking more of your fantastic post. Also, I’ve shared your website in my social networks!
excellent submit, very informative. I wonder why the other experts of this sector do not realize this. You should proceed your writing. I’m confident, you have a huge readers’ base already!