This week the changes in the development of your baby are exciting, at 21 weeks you are officially in the second half of your pregnancy. Today we are going to talk about your 21 week baby ultrasound. As usual, you are going to find ultrasound images combined with everything you need to know about your 21 week pregnancy in this post, so let’s begin…
How Big Is your Baby at 21 Weeks Pregnant?
At 21 weeks pregnant, the baby is as big as a Pomegranate. The average 21 week fetus weighs about 12.7 ounces and measures 10.5 inches long.
Your baby is big enough now that you’ve probably been feeling his or her fetal movements more and more lately.

Your 21 Weeks Pregnant Symptoms.
Braxton Hicks contractions: You might start noticing mild contractions at this point. Some patients more than others, Braxton hicks contractions is when your uterus occasionally feel tight as it practices for labor. This is totally normal as long as the contractions go away when you change positions. Let your doctor know about any pain or contractions that don’t stop, Keep in mind that Dehydration can cause Premature Labor. So try to keep yourself hydrated at all times. If you are pregnant with twins expect to be feeling more of this contractions.
Stretch marks: Stretch marks are a form of scarring on the skin. Over time they may diminish. But will not disappear completely. Stretch marks usually form during the second and third trimester, and usually on the belly, but also can occur on the breasts, thighs, hips, lower back and buttocks. These are known as striae gravidarum. Stretch marks are more common for some women simply because of family history, lack on collagen or because of sudden weight gain.
Dry, itchy skin: Your skin is stretching over your growing bump, making it more irritated by the day. Using a pregnancy safe body oil or lotion will help your skin stay moisturized and hopefully less itchy. Also, if you develop a rash, let your doctor know right away.
Leaky boobs: Your milk ducts will be fully developed by the end of this trimester just in case of early arrival.
Heartburn and/or indigestion: Avoid spicy and greasy foods and other triggers. If the source of your discomfort is a mystery, keeping a food diary could help you figure it out.
I want to remind you that other symptoms such as Vaginal discharge, Hip pain, and Abdominal aches might be part of your normal second-trimester list of symptoms. All normal and part of the process of growing a baby in your uterus, try to rest when you have the chance, stay hydrated, try to have a healthy and balanced diet, and give yourself a lot of love.
Pin it here!
Helpful related post: How to deal with gestational diabetes for a healthier pregnancy.
Fetal development at 21 weeks.
- Baby’s Taste Buds Develop: When you’re 21 weeks pregnant, your baby is swallowing amniotic fluid each day not only for nutrition and hydration but also to practice swallowing and digesting. Skills he’ll need as soon as he arrives.
- Baby’s Getting Coordinated: Arms and legs are finally in proportion. Neurons are now connected between the brain and muscles, and cartilage throughout the body is turning to bone. All these developments give to your baby more control over limb movements, which explains all that kicking and stretching you may have started feeling.
- The reproductive system is developing too: If it’s a girl, she’s already got a lifetime supply of eggs in her womb about six million of them. If its a boy. His testes are still located in his abdomen but will drop in the coming weeks once the scrotum finishes developing.
What to know about doctor visits.
Your doctor will measure the fundal height at each prenatal visit at this point. Fundal height is the distance from the pubic bone to the top of your uterus. In centimeters, the fundal height should match your week of pregnancy, give or take two centimeters.
It should continue to increase about a centimeter each week. A higher or lower fundal height could be the sign of a pregnancy condition such as gestational diabetes, a growth issue, or a breech baby, so if it doesn’t appear to be average, further testing may be necessary.
If there is any questionable size discrepancy then Ultrasound is the way to go to check fetal growth.
At this point, Ultrasound is only done under certain circumstances, only if you are experiencing Pelvic pressure, Pelvic pain, vaginal bleeding and/or vaginal discharge.
Ultrasound Protocol at 21 weeks might include:
- Biparietal Diameter( BPD )
- Head circumference( HC )
- Abdominal circumference( AC )
- Femur length( FL )
- Measurements on the Amniotic Fluid levels are also done.
- Checking out Placenta again, Anterior or Posterior Placenta is fine as long as the placenta isn’t Previa ( covering cervical canal ) is all fine.
Ultrasound doesn’t need to check again major organs and intracranial structures because that was already done on the Anatomy Scan.
Normal 21 week baby ultrasound images.
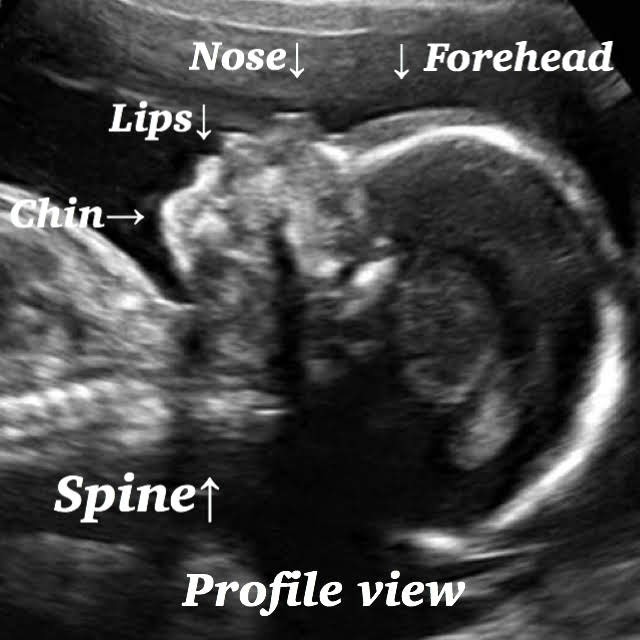
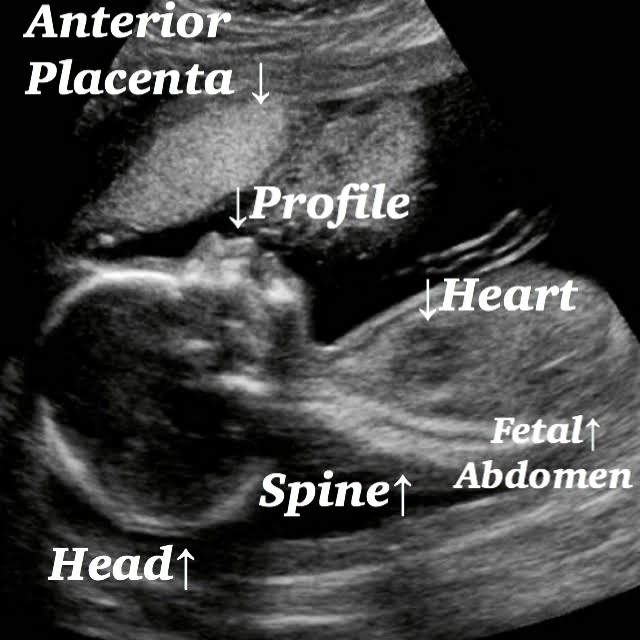
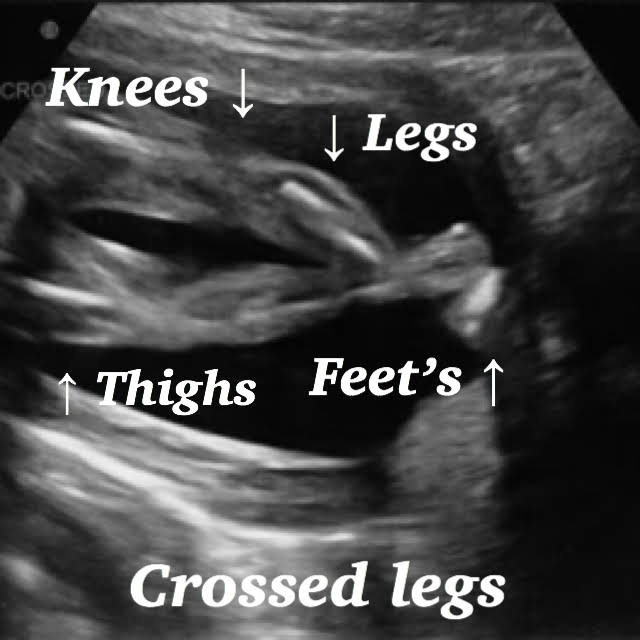
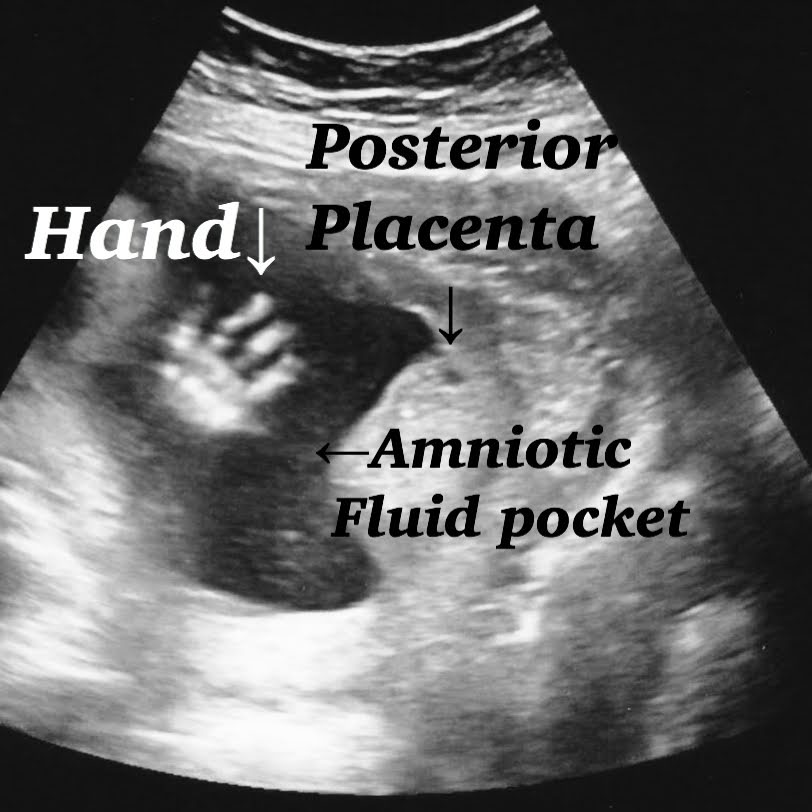
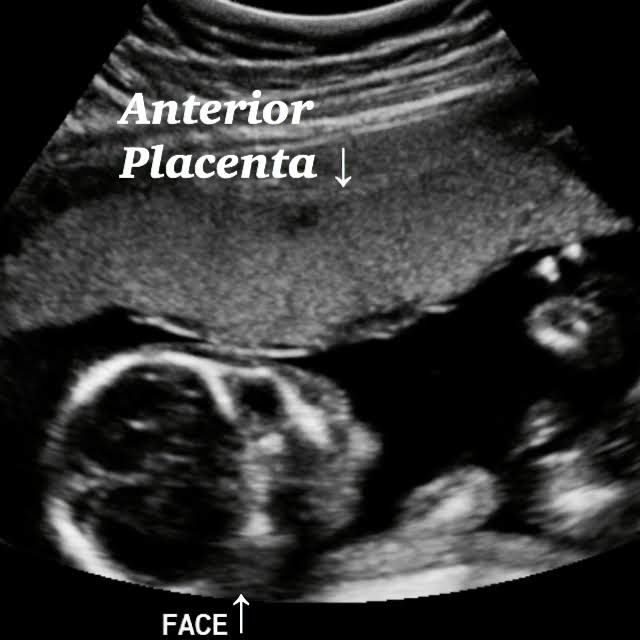
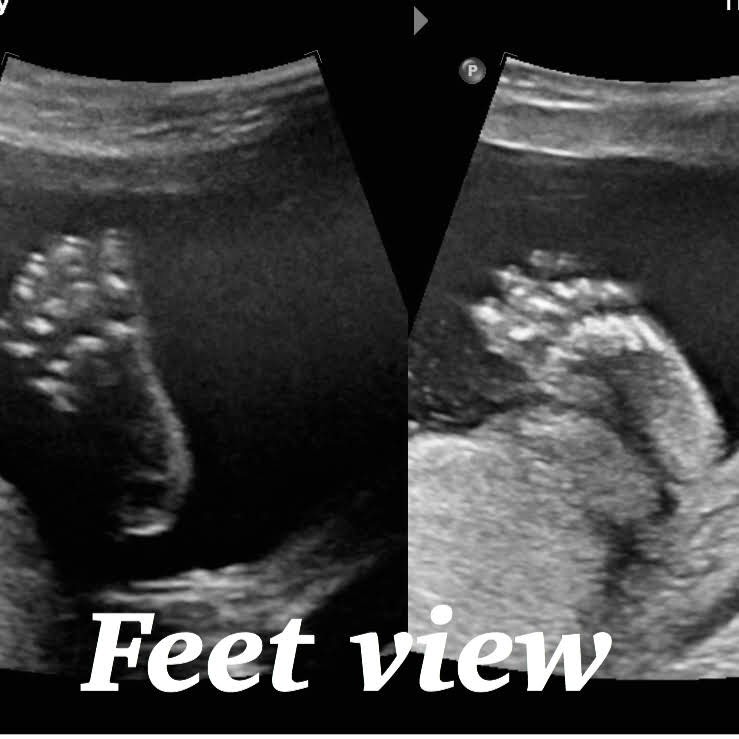
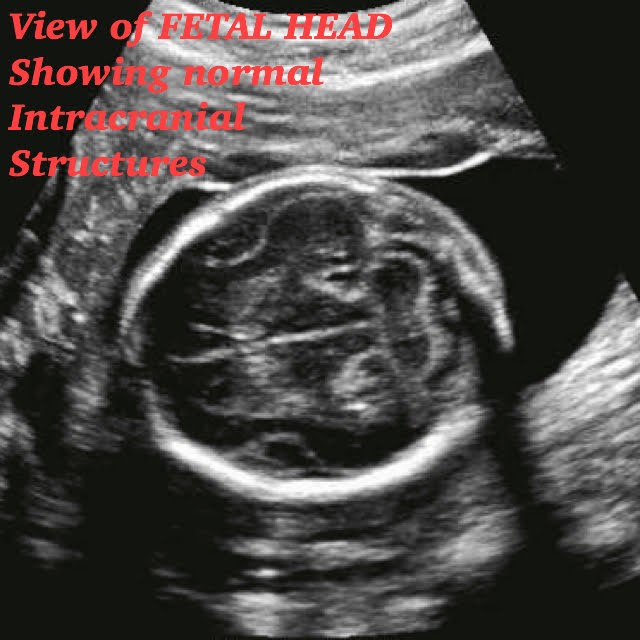
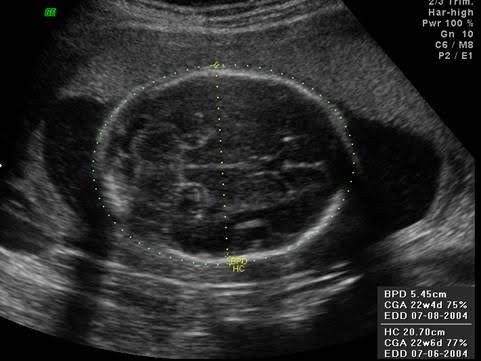
Fetal head
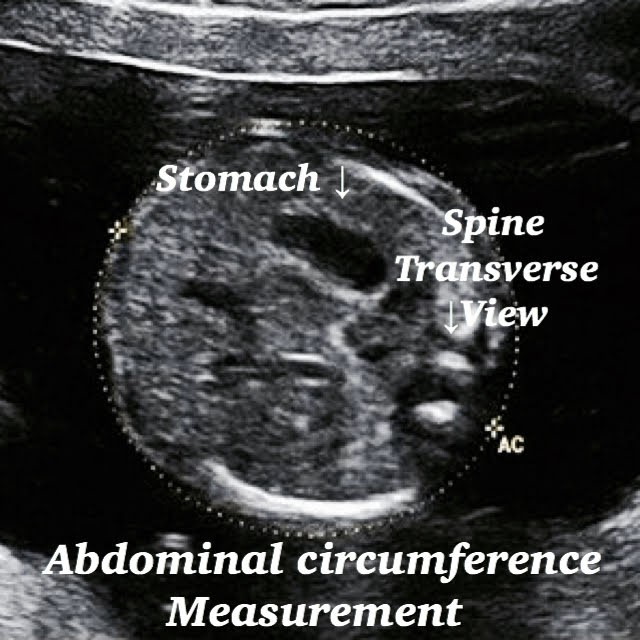
Abdominal circumference.
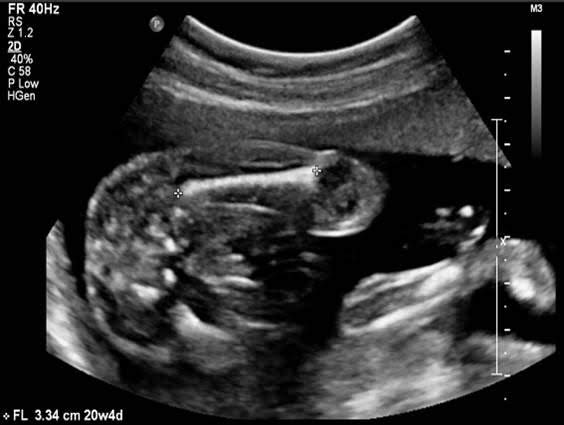
Femur
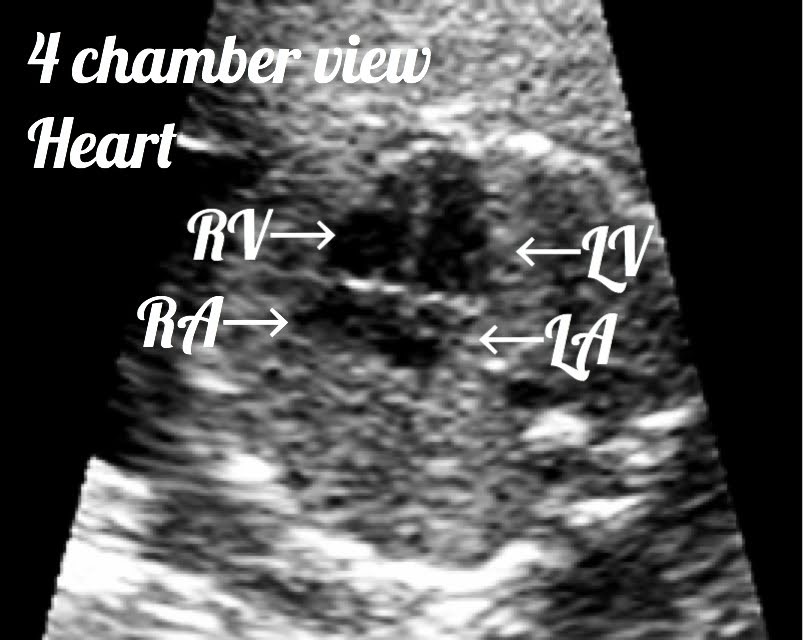
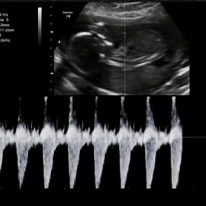
Normal fetal heart rate should be between 120 to 170 bpm.
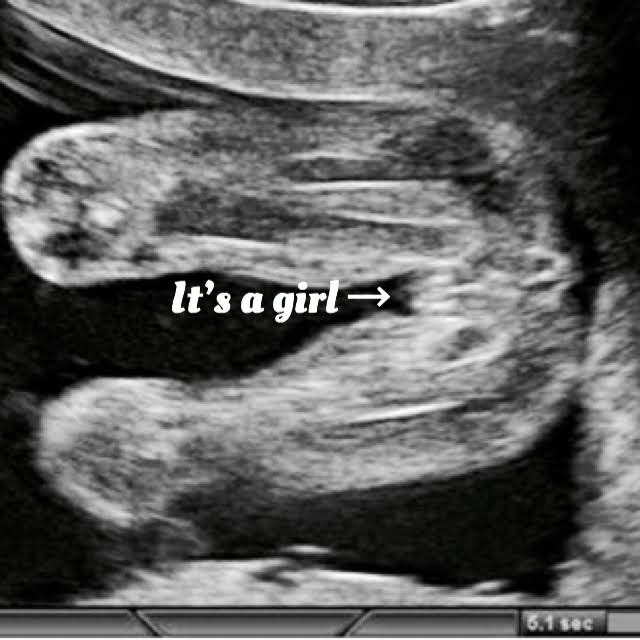
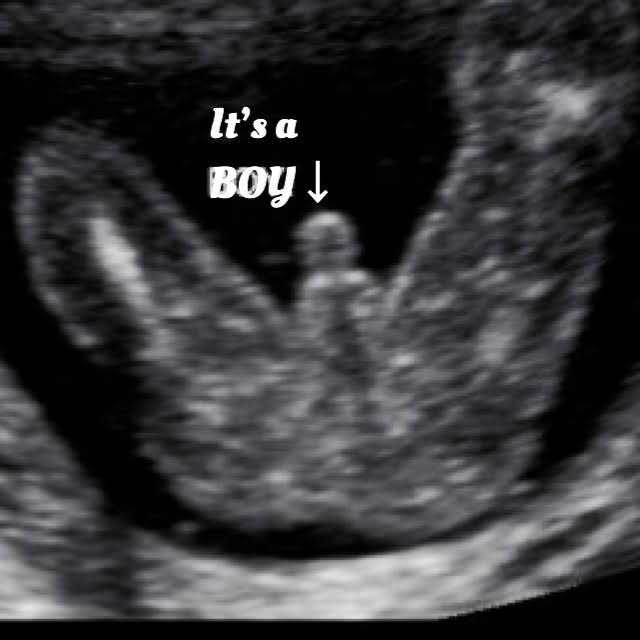
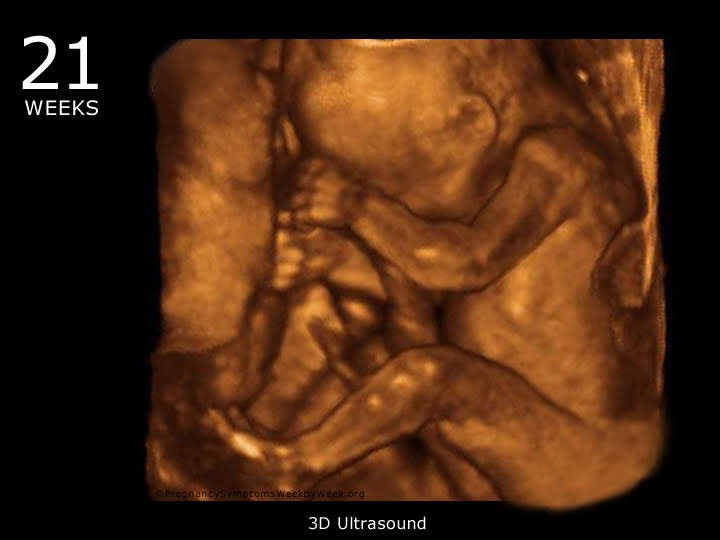 :
:
Final thoughts about 21 week baby ultrasound.
This is the most important information about your 21 week baby ultrasound, pregnancy, fetal development and doctor visit. I hope this post was helpful to you. In my next post I will be talking about 22 week pregnancy and ultrasound, thanks for visiting my blog today, I will see you next time.
Zadi. xo
Disclaimer: Due to HIPPA compliance and regulations all patient information is protected on this site. Also, the information provided on my blog is designed to provide helpful information about the topic and are made with the best of my knowledge, therefore, is not intended to diagnose or treat any medical condition, For diagnosis or treatments on any medical problems consult your own physician. The author is not responsible or liable for any mistreated pathologies or wrong treatments.










It’s been so long since I’ve looked at ultrasounds of babies… Amazing imagery today! Great, informative article.
Thanks dear, I highly appreciate your comments, coming from a colleague ?
My pleasure!
Wonderful post
Thanks ?
Thanks, I am glad you think so ?
You will
[…] The ultimate guide for your 21 week ultrasound. […]